-
Colorectal and Small Bowel Tumor SurgeryOpen or Close
resecting (removing) the tumor and a section of the affected intestine, along with nearby lymph nodes, to check for cancer spread.
-
Diverticular DiseaseOpen or Close
Diverticular disease- A condition in which small, bulging pouches develop in the digestive tract.
-
ConstipationOpen or Close
Constipation- a condition in which there is difficulty in emptying the bowels, usually associated with hardened feces.
-
Rectal ProlapseOpen or Close
Rectal Prolapse- The lining (mucous membrane) of the rectum slides out of place and usually sticks out of the anus.
-
Colostomy and Ileostomy SurgeryOpen or Close
surgical procedures that create an opening (stoma) in the abdomen to divert waste products from the digestive system to an external bag. .
-
Colovaginal and Colovesicular FistulasOpen or Close
typically involves the resection (surgical removal) of the affected section of the colon and primary anastomosis (reconnecting the healthy ends of the colon). For colovesical fistulas, the bladder wall is also repaired.
-
Laparoscopic gallbladder surgeryOpen or Close
During a laparoscopic cholecystectomy, the surgeon makes four small incisions in your abdomen. A tube with a tiny video camera is inserted into your abdomen through one of the incisions. Your surgeon watches a video monitor in the operating room while using surgical tools inserted through the other incisions in your abdomen to remove your gallbladder.
Next you may undergo an imaging test, such as an X-ray or ultrasound, if your surgeon is concerned about possible gallstones or other problems in your bile duct. Then your incisions are sutured, and you're taken to a recovery area. A laparoscopic cholecystectomy takes one or two hours.
A laparoscopic cholecystectomy isn't appropriate for everyone. In some cases your surgeon may begin with a laparoscopic approach and find it necessary to make a larger incision because of scar tissue from previous operations or complications. -
Laparoscopic ventral, umbilical, and incisional hernia repairOpen or Close
Laparoscopic ventral hernia repair is a technique to fix tears or openings in the abdominal wall using small incisions, laparoscopes (small telescopes inserted into the abdomen) and a patch (screen or mesh) to reinforce the abdominal wall. It may offer a quicker return to work and normal activities with decreased pain for some patients.
An umbilical hernia occurs when a tissue bulges out through an opening in the muscles on the abdomen near the navel or belly button (umbilicus). About 10% of abdominal hernias are umbilical herniasThe hernia is repaired with mesh or sutures inserted through instruments placed into small incisions in the abdomen.
An incisional hernia is a type of hernia caused by an incompletely-healed surgical wound. Since median incisions in the abdomen are frequent for abdominal exploratory surgery.
-
Complex hernia surgeryOpen or Close
A hernia becomes complex when repeated surgical attempts to close the hole in the abdominal wall fail. In cases where hernia surgery fails and the person has a recurrent hernia, the chances of the surgery being successful diminish with each successive surgery. When surrounding tissue is especially weak or stretched, it may need to be augmented or replaced. This often occurs in areas of previous surgical scars, the umbilicus, or in the groin area.
-
Recurrent hernia surgeryOpen or Close
A recurrent hernia is the result of an unsuccessful hernia repair. It is characterized by return of the bulge at or near the site of the previous hernia. It can sometimes present itself with pain, and in the event of intestines within the recurrent hernia sac, it may present with nausea and vomiting.
-
Laparoscopic appendectomyOpen or Close
The words “laparoscopic” and “open” appendectomy describes the techniques a surgeon uses to gain access to the internal surgery site. Most laparoscopic appendectomies start the same way. Using a cannula (a narrow tube-like instrument), the surgeon enters the abdomen. A laparoscope (a tiny telescope connected to a video camera) is inserted through a cannula, giving the surgeon a magnified view of the patient’s internal organs on a television monitor. Several other cannulas are inserted to allow the surgeon to work inside and remove the appendix. The entire procedure may be completed through the cannulas or by lengthening one of the small cannula incisions. A drain may be placed during the procedure. This will be removed later by your surgeon.
-
Soft tissue tumor excisionOpen or Close
The vast majority of benign soft tissue tumors can be treated with a single clean surgical procedure and minimal risk to surrounding normal blood vessels, nerves, muscle or bone.
-
Parastomal Hernia RepairsOpen or Close
Parastomal hernia repairs- is a type of incisional hernia that allows protrusion of abdominal contents through the abdominal wall defect created during ostomy formation.
-
Laparoscopic inguinal and femoral hernia repairOpen or Close
Inguinal hernias are common among men; one in four men develops an inguinal hernia during his lifetime, and that likelihood increases with age. They emerge at the inguinal canal, through which the spermatic cord, several nerves and vessels travel. These structures are slightly above the groin crease. The majority of inguinal hernia cases involve one side of the body only, although a hernia can be present on the other side without signs or symptoms.
Femoral hernias are significantly rarer and emerge relatively more frequently in women because of the different anatomy of the pelvis. They emerge at the femoral canal, through which the femoral vein, artery and nerve travel from the abdomen to the leg; these structures lie slightly below the groin crease. Pain may be felt at the groin and upper thigh. With these hernias, the sac of small intestine is more often incarcerated – it cannot be pushed back through the defect in the fascia – or strangulated, cutting off blood supply to the small intestine, although this is still rare.
-
Gastric and small bowel tumor resectionOpen or Close
A small bowel resection is the removal of part of the small intestine. The small intestine includes the duodenum, jejunum, and ileum. The surgery can be done through an open incision or using smaller incisions using a laproscope.
-
Laparoscopic colon resectionOpen or Close
A technique known as minimally invasive laparoscopic colon surgery allows surgeons to perform many common colon procedures through small incisions. Depending on the type of procedure, patients may leave the hospital in a few days and return to normal activities more quickly than patients recovering from open surgery.
In most laparoscopic colon resections, surgeons operate through 4 or 5 small openings (each about a quarter inch) while watching an enlarged image of the patient’s internal organs on a television monitor. In some cases, one of the small openings may be lengthened to 2 or 3 inches to complete the procedure.
-
Laparoscopic feeding tube placementOpen or Close
Laparoscopic Gastrostomy or Jejunostomy. The surgeon will make about 2-3 small incisions in your abdomen. A port (nozzle) is inserted into one of the slits, and carbon dioxide gas inflates the abdomen. This process allows the surgeon to see inside of your abdomen more easily. A laparoscope is inserted through another port. The laparoscope looks like a telescope with a light and camera on the end so the surgeon can see inside the abdomen. Surgical instruments are placed in the other small openings and used to place the feeding tube into your stomach (gastrostomy) or small bowel (jejunostomy). Your doctor will discuss with you before surgery the best place to place the feeding tube. The tube will exit out of your skin, and will be temporarily held in place with four stitches that are attached to half-inch white bolsters on your skin. These stitches will be removed several weeks after surgery. After the tube has been placed, the carbon dioxide is released out of the abdomen through the slits, and then these sites are closed with sutures or staples, or covered with glue-like bandage and steri-strips.
-
Laparoscopic peritoneal dialysis catheter placementOpen or Close
The surgeon will make about 2-3 small incisions in your abdomen. A port (nozzle) is inserted into one of the slits, and carbon dioxide gas inflates the abdomen. This process allows the surgeon to see inside of your abdomen more easily. A laparoscope is inserted through another port. The laparoscope looks like a telescope with a light and camera on the end so the surgeon can see inside the abdomen. Surgical instruments are placed in the other small openings and used to place the peritoneal dialysis catheter into your abdominal cavity. The catheter will exit out of your skin. After the catheter has been placed, the carbon dioxide is released out of the abdomen through the slits, and then these sites are closed with sutures or staples, or covered with glue-like bandage and steri-strips.
-
Implantable center venous access portOpen or Close
The port is surgically implanted beneath the skin, and generally in the chest region. The incision is made halfway between the clavicle and nipple on either the left or right side of the chest. The right side of the chest is generally preferred since the anominate vein curves down more directly to the superior vena cava (SVC). The surgeon makes the final decision about the site for implantation based on skin condition, presence of a pacemaker, and taking into account other medical conditions that would contra-indicate the use of a particular site. An approximate 5-cm incision in the skin is made at the selected site. A “kangaroo” pocket is created approximately two inches away from the incision line and 0.5-cm to 2.0 cm deep into which the portal body is placed. The pocket is located away from the incision line in order to avoid rupturing the incision with subsequent accessing of the port. The I.P. is placed in this pocket and sutured in place to the underlying tissue.
-
Temporal artery biopsyOpen or Close
A temporal artery biopsy is a procedure in which a small piece of tissue is removed from your temporal artery and then studied under a microscope to check for signs of inflammation and damage.
-
Skin and soft tissue tumor resectionOpen or Close
Excision of subcutaneous soft tissue tumors involves the simple or marginal resection of tumors confined to subQ tissue below the skin but above the deep fascia 5· There are 3 layers of fascia- superficial fascia/subQ tissue, deep fascia, and subserous fascia· The superficial fascia / subQ tissue is located directly under the subcutis of the skin. Its functions include the storage of fat and water and it also provides passageways for nerves and blood vessels. In some areas of the body it also houses a layer of skeletal muscle, allowing for movement of the skin. SubQ tissue tumors are usually benign and are resected without removing a significant amount of surrounding normal tissue.
-
Melanoma excisionOpen or Close
Surgery to remove (excise) a melanoma removes the entire melanoma along with a border (margin) of normal-appearing skin. The width of the border of normal skin removed depends on the depth of the melanoma. More tissue, usually skin and fat, is also removed from under the melanoma.
-
Abscess and skin infection drainageOpen or Close
A doctor will cut into the lining of the abscess, allowing the pus to escape either through a drainage tube or by leaving the cavity open to the skin. How big the incision is depends on how quickly the pus is encountered.
Once the abscess is opened, the doctor will clean and irrigate the wound thoroughly with saline. If it is not too large or deep, the doctor may simply pack the abscess wound with gauze for 24-48 hours to absorb the pus and discharge.
-
Skin graftsOpen or Close
Skin grafting is a type of graft surgery involving the transplantation of skin. The transplanted tissue is called a skin graft.
-
Laparoscopic sleeve gastrectomyOpen or Close
During the procedure about 85% of the left side of the stomach is removed, leaving only a thin tube-like sleeve of stomach about the diameter of your index finger. The sleeve is similar in shape to a hot dog. Removing most of the stomach limits the amount of food you can eat and helps you feel full quicker.
The portion of the stomach that is removed also normally produces a hunger hormone known as ghrelin. Removing this portion of your stomach decreases this appetite-stimulating hormone and as a result generally decreases appetite. Because there are no further anatomical rearrangements, the sleeve allows for normal digestion and absorption. Unlike other procedures that rearrange the intestines, with the sleeve there is minimal risk of patients developing protein and vitamin deficiencies
-
Laparoscopic gastric bypassOpen or Close
The "Roux-en-Y gastric bypass" (RYGB) is considered the "gold standard" for weight-loss surgery by the American Society for Metabolic and Bariatric Surgery and the National Institutes of Health. RYGB works by restricting food intake and by decreasing the absorption of food. Food intake is limited by a small pouch that is similar in size to the adjustable gastric band. In addition, absorption of food in the digestive tract is reduced by excluding most of the stomach, duodenum, and upper intestine from contact with food by routing food directly from the pouch into the small intestine. The operation, usually performed laparoscopically, involves making five to six small incisions in the abdomen through which a small scope connected to a video camera and surgical tools are inserted. The surgeon staples the top portion of the stomach so it is separated from the bottom to create a small stomach pouch. This small pouch restricts food intake. A section of the small intestine called the jejunum is then attached to the small stomach pouch permitting food to bypass the lower stomach, the duodenum. This bypass reduces the amount of calories and nutrients the body absorbs, called malabsorption.
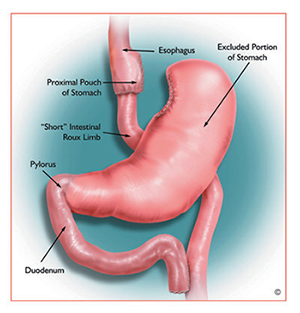
In the graphic above, the outlet from the new small stomach pouch empties directly into the lower portion of the small intestine, called the jejunum, thus bypassing calorie absorption. This is done by dividing the small intestine just beyond the duodenum to connect it with the newly formed stomach pouch. The other end is connected to the side of the Roux limb of the intestine creating a "Y" shape that gives the technique its name. The length of either segment of the intestine can be increased to produce some degree of malabsorption.
Advantages
1. Average weight loss after the Roux-en-Y procedure is generally higher if you rigorously follow instructions than with other restrictive procedures.
2. A year after surgery, weight loss averages 77 percent of excess body weight.
3. Studies show that after 10 to 14 years, 50 percent to 60 percent of excess body weight loss is maintained by some patients.
4. A study of 500 patients, conducted in 2000, showed that 96 percent of certain health conditions -- including back pain, sleep apnea, high blood pressure, diabetes and depression -- were improved or resolved.
Disadvantages
1. Because the duodenum is bypassed, poor absorption of iron and calcium can result in the lowering of total body iron, which may result in iron deficiency anemia. Metabolic bone disease has also occurred in some patients.These can be managed through proper diet and vitamin supplements.
2. Chronic anemia due to Vitamin B12 deficiency may occur. This problem usually can be managed with Vitamin B12 pills or injections.
3. A condition known as "dumping syndrome" can occur as the result of rapid emptying of stomach contents into the small intestine. This is sometimes triggered when too much sugar or large amounts of food are consumed.
4. In some cases, the procedure's effectiveness may lessen if the stomach pouch is stretched or if it is initially left larger than 15 to 30 cubic centimeters.
5. The bypassed portion of the stomach, duodenum and segments of the small intestine cannot be easily visualized using X-ray or endoscopy if problems such as ulcers, bleeding or malignancy occur.
-
Lap band removalOpen or Close
Lap band removal-As part of Lap-Band removal, the surgeon needs to cut the capsule created by the body around the device, remove sutures and any scar tissue formed, as well as the band itself. The band, tube and port will then be removed from the stomach through the incision. If the patient was initially submitted to a laparoscopic procedure, the removal surgery can be performed using the same incisions initially created and will take about 10 minutes.
-
Revisional bariatric surgeryOpen or Close
Revisional Bariatric Surgery- Revising bariatric surgery refers to a secondary procedure that is performed after the initial bariatric surgery either involved complications or was not successful.
-
Laparoscopic splenectomyOpen or Close
Lap Spleenectomy-Splenectomy is a surgical procedure to remove your spleen. The spleen is an organ that sits under your rib cage on the upper left side of your abdomen. Splenectomy is most commonly performed using a tiny video camera and special surgical tools.
-
Laparoscopic feeding tube placement (gastric, jejunum)Open or Close
Lap Feeding Tube Placement- A gastrostomy tube, also known as “g-tube”, is a small feeding tube that is placed in the stomach for feeding or decompression. G-tubes are placed surgically or straight through the skin (percutaneously). Surgical placement is either laparoscopic or open and can accompany other procedures.
-
Laparoscopic surgery for benign and milignant gastric tumorsOpen or Close
Lap surgery for benign/malignant gastric tumors- Laparoscopic distal gastrectomy with gastrojejunostomy is done for tumors of the pylorus. A combined laparoscopic-endoscopic approach allows precise localization of the lesion by direct visualization. Laparoscopic resection of benign gastric tumors is a reliable and safe method as shown by data in the literature.
-
Laparoscopic surgery for gastric cancerOpen or Close
Lap surgery for gastric cancer- a minimally invasive procedure in which the surgeon removes the stomach while guided by a magnified image projected by a thin, lighted tube with a video camera at its tip, called a laparoscope.
-
Laparoscopic surgery for gastroparesis (gastric pacemaker)Open or Close
Lap surgery for gastric pacemaker- provide mild electrical stimulation to the lower stomach nerves. Transmitted through a neurostimulator, these mild electrical pulses encourage the stomach to contract and help to relieve nausea and vomiting. Utilizing minimally invasive surgical techniques, the gastric pacemaker is placed subcutaneously below the rib cage in the abdomen.
-
Laparoscopic fundoplication (Nissen)Open or Close
Lap Fundoplication- A Nissen fundoplication, or laparoscopic Nissen fundoplication when performed via laparoscopic surgery, is a surgical procedure to treat gastroesophageal reflux disease (GERD) and hiatal hernia.
-
Laparoscopic surgery for achalasia (Heller myotomy)Open or Close
Lap Surgery Achalasia- A surgical procedure called the Heller myotomy has become the treatment of choice and offers long-term symptomatic relief to those who have the disorder. This procedure destroys the muscles at the gastroesophageal junction, allowing the valve between the esophagus and stomach to remain open .
-
Laparoscopic Hiatel and Paraesophageal hernia repairOpen or Close
Laparoscopic Cruroplasty and Nissen fundoplication is the procedure of choice for repair of a hiatal hernia. Patients that have paraesophageal hernia which allows the fundus to be displaced into the chest above the GE junction or patients with other abdominal organs (e.g. spleen, colon, liver) displaced into the chest should be repaired urgently. Repair will help prevent complications such as bleeding, intestinal disruption, strangulation and the like. Elective repair is recommended only for patients that are asymptomatic and have a sliding hernia. This group of asymptomatic patients may also be followed clinically seeking surgery only when symptoms arise.
In the past, open surgery was the only option for repair. This approach is associated with prolonged recovery time and a large painful incision. With the new minimally invasive approach, surgery is now a viable initial therapy even for patients who are asymptomatic. The laparoscopic cruroplasty and Nissen fundoplication is performed through five quarter-inch incisions through which, a camera and instruments are placed. The hernia is reduced from the chest into the abdomen. This may require separation of abdominal organs from the lung and middle chest structures.
The hiatus is then re-approximated to the appropriate size. Some hernias are so large and tissues are so poor that prosthetic material must be used to prevent recurrence. After adequate repair of the hiatus, a new lower esophageal valve is constructed by wrapping a two-centimeter portion of the stomach around the lower most portion of the esophagus. This collar is then anchored to the tough fibers of the diaphragm. The procedure typically lasts for two to four hours depending on the size and contents of the hernia. Patients are started on clear liquids the next morning and are discharged in the afternoon. The open surgical technique involves an 8-10 inch upper abdominal incision with a hospital stay of 5-7 days.
-
Partial and total thyroidectomyOpen or Close
A thyroidectomy is an operation that involves the surgical removal of all or part of the thyroid gland. Head and Neck or Endocrine Surgeons often perform a thyroidectomy when a patient has thyroid cancer or some other condition of the thyroid gland (such as hyperthyroidism) or goiter. Other indications for surgery include cosmetic (very enlarged thyroid), or symptomatic obstruction (causing difficulties in swallowing or breathing). Thyroidectomy is a common surgical procedure that has several potential complications or sequelae including: temporary or permanent change in voice, temporary or permanently low calcium, need for lifelong thyroid hormone replacement, bleeding, infection, and the remote possibility of airway obstruction due to bilateral vocal cord paralysis.
-
Parathyroidectomy and subtotal parathyroidectomyOpen or Close
Parathyroidectomy is the removal of one or more of the parathyroid glands. The parathyroid glands are usually four in number, although the exact number may vary from three to seven. They are located in the neck in front of the Adam's apple and are closely linked to the thyroid gland. The parathyroid glands regulate the balance of calcium in the body.
Parathyroidectomy is usually done to treat hyperparathyroidism (abnormal over-functioning of the parathyroid glands).
-
Laparoscopic adrenal resectionsOpen or Close
The laparoscopic approach for adrenal resection allows small to moderately sized tumors to be removed using scopes and very small incisions.
-
Fine needle aspiration biopsy (FNA)Open or Close
Fine needle aspiration is a type of biopsy procedure. In fine needle aspiration, a thin needle is inserted into an area of abnormal-appearing tissue or body fluid. As with other types of biopsies, the sample collected during fine needle aspiration can help make a diagnosis or rule out conditions such as cancer.
-
Total mastectomyOpen or Close
The entire breast is removed, but no lymph nodes are taken in this procedure. Simple mastectomy is most frequently used for further cancer prevention or when the cancer has not spread to the lymph nodes.
-
LumpectomyOpen or Close
Lumpectomy (also known as breast conserving surgery, partial mastectomy or wide excision) is a surgery to remove cancer from the breast. Unlike a mastectomy, a lumpectomy removes only the tumor and a small rim of normal tissue around it. It leaves most of the breast skin and tissue in place.
-
Axillary lymph node dissectionOpen or Close
Surgery to remove lymph nodes from the armpit (underarm or axilla). The lymph nodes in the armpit are called axillary lymph nodes. An ALND is also called axillary dissection, axillary node dissection or axillary lymphadenectomy.
-
Sentinel lymph node biopsyOpen or Close
A sentinel lymph node biopsy (SLNB) is a procedure in which the sentinel lymph node is identified, removed, and examined to determine whether cancer cells are present. A negative SLNB result suggests that cancer has not developed the ability to spread to nearby lymph nodes or other organs.
-
Breast conserving surgeryOpen or Close
Breast-conserving surgery is a less radical cancer surgery than mastectomy. Breast-conserving surgery, as in a lumpectomy removes part of the breast tissue during surgery, as opposed to the entire breast.
-
Surgical breast biopsyOpen or Close
The tissue removed during a biopsy is studied under a microscope to see if cancer is present. If cancer is found, other tests are done on the tissue to help plan your treatment.